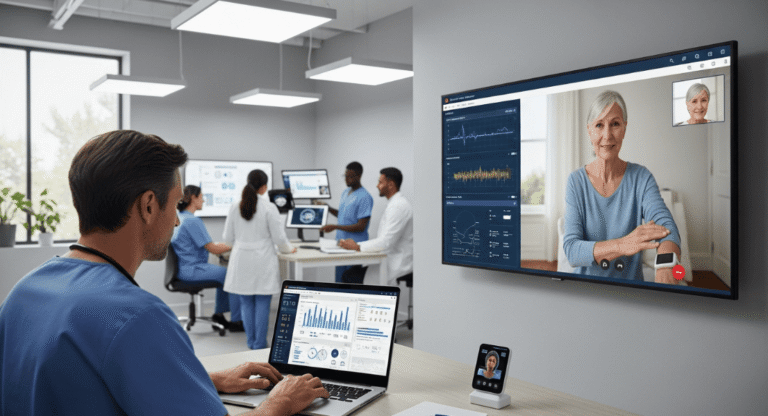
Healthcare providers use CPT Code 99490 for chronic care management services. This code covers non-face-to-face care for patients with chronic conditions. These services support patients outside regular clinical visits. Providers aim to improve long-term patient health outcomes. Providers use this code for ongoing monitoring and care coordination. This code mainly applies to patients with multiple chronic conditions.
Understanding Chronic Care Management Services
Chronic care management focuses on long-term patient care. It helps patients manage complex health conditions more effectively. Care teams provide coordination and regular follow-up support. They also perform medication review and patient education services. Healthcare teams work together to improve patient health outcomes. This approach helps reduce hospital visits and complications.
Patient Eligibility Criteria for CPT 99490
Providers cannot enroll every patient in this service. They must follow specific criteria before billing begins. The patient must have at least two chronic conditions. These conditions must last at least twelve months or longer. These conditions must place the patient at significant health risk. These risks include decline or possible hospitalization. Providers must obtain patient consent before starting services.
Time Requirements for Billing CPT 99490
Providers must track time carefully for this code. They must meet the required minimum time threshold. Clinical staff must provide at least twenty minutes each month. Providers must direct this clinical staff work. Providers can count only non-face-to-face services. They must maintain accurate and consistent time records. Providers risk claim denial if they miss time requirements.
Provider Responsibilities in CCM Services
Providers must ensure proper and continuous care delivery. They oversee clinical staff involved in care management services. Providers must create and maintain a comprehensive care plan. They should include patient history and clear treatment goals. Providers must ensure ongoing access to care management services. They should coordinate with other healthcare professionals when needed. Providers must use secure systems for sharing patient information.
Documentation Requirements for CPT Code 99490
Providers must maintain complete and accurate documentation. This documentation supports compliance and reduces audit risks. Providers must record the total time provided each month. They must clearly document all delivered services. Providers must record and retain patient consent properly. They should update care plans based on patient needs. Providers must document all patient communication activities. Incomplete documentation can lead to claim rejection.
Billing Guidelines and Reimbursement Process
Providers can bill CPT 99490 once per calendar month per patient. Only one practitioner can bill this service each month. Medicare determines reimbursement through the Physician Fee Schedule. Payers adjust payment based on geographic and policy factors. Providers must use the correct place-of-service codes when required. They must follow payer-specific billing guidelines carefully. Providers should verify payer rules to prevent billing errors.
Difference Between CPT 99490 and Other CCM Codes
Healthcare systems use several related chronic care management codes.
Each code depends on the time spent and service complexity.
CPT 99490 covers standard chronic care management services.
It requires at least twenty minutes of monthly service time.
Providers use CPT 99487 for complex chronic care management.
This code involves higher levels of medical decision-making.
Providers use CPT 99439 for each additional twenty minutes.
Providers must select the correct code for accurate billing.
Common Conditions Covered Under CPT 99490
Many chronic conditions qualify for this management service. These conditions require long-term, continuous care support. Providers commonly manage diabetes and hypertension under this code. They also include heart disease and asthma in many cases.Providers frequently manage arthritis and chronic lung diseases. These conditions often require ongoing monitoring and management.Providers must use accurate diagnosis coding for proper billing.
Compliance and Regulatory Requirements
Providers must follow strict compliance in medical billing practices. They must follow established regulatory and payer guidelines. Providers must obtain patient consent before services begin. They must ensure that only one provider bills each month. Providers must maintain accurate documentation at all times. They must keep time tracking clear and verifiable. Providers may face audits or penalties for non-compliant billing.
Common Billing Errors and How to Avoid Them
Billing errors can reduce revenue and increase claim denials. Providers can avoid many errors with proper staff training. Providers often fail to meet required time thresholds. They also miss proper documentation of patient consent. Incomplete documentation often leads to claim rejection. Incorrect code selection also creates billing issues. Providers should conduct regular internal audits to fix errors.
Benefits of CPT Code 99490 for Providers and Patients
If the healthcare providers can use the CPT code 99490 effectively, they can avail the multiple benefits from this code.
- It supports a recurring monthly revenue opportunity.
- It also improves patient engagement and care coordination.
- Providers can deliver more consistent and proactive care.
- Patients receive continuous support for chronic conditions.
- This support may reduce emergency visits and complications
- Consistent monitoring can improve overall patient outcomes.
Best Practices to Improve CCM Services
Providers should follow best practices for better outcomes.
- Structured workflows help improve service quality and efficiency.
- Staff training improves documentation accuracy and compliance.
- Time tracking tools help maintain proper service records.
- Providers should communicate regularly with patients.
- They should review and update care plans consistently.
Role of Technology in Chronic Care Management
Technology plays an important role in CCM services. It improves efficiency and accuracy in care delivery processes. Electronic health records help providers store patient data securely. They allow quick access to a complete medical history.
Remote monitoring tools support ongoing patient assessment. They help providers identify health concerns early. Communication tools improve interaction between providers and patients.
Internal Linking Opportunities
You can strengthen SEO performance through internal linking.
Anchor Text: Infectious disease ICD 10 codes
https://www.icd10data.com/ICD10CM/Codes/A00-B99/B00-B09
Anchor Text Viral infection ICD 10 classification
https://www.icd10data.com/ICD10CM/Codes/A00-B99/B25-B34
Conclusion
CPT Code 99490 supports structured chronic care management services. It allows providers to manage patients outside of in-person visits. Providers must maintain accurate documentation and time tracking. They must follow billing rules to ensure correct reimbursement. This code benefits both providers and patients significantly. It supports better care delivery and improved health outcomes.